|
In addition, we systematically review cases reported in the literature to provide information on the clinical symptoms, magnetic resonance imaging (MRI) findings, electroencephalographic (EEG) abnormalities, and treatment and prognosis of this rare overlap syndrome. This paper reports a case of FLAMES combined with anti-NMDARe. In addition, Martinez-Hernandez ( 5) reported that patients with anti-NMDARe combined with MOG-Ab positivity have additional clinical radiological characteristics that may affect prognosis.ĭespite previous case reports on the coexistence of FLAMES with anti-NMDARe, the clinical features, ancillary tests, treatment, and prognosis of these combined conditions have not been reviewed in detail. A study of 215 anti-NMDARe patients, in which only 22 patients were positive for MOG-Ab, concluded that double antibody positivity is rare ( 4). Between 4% and 7.5% of patients with anti-NMDARe have both glial and neuronal surface antibodies. Patients may experience abnormal mental behavior, involuntary movements of the mouth, and central hypoventilation. Atypical manifestations of demyelination, such as fever, headache, epilepsy, and aphasia, are common in FLAMES.Īnti-NMDAR encephalitis is one of the most common types of autoimmune encephalitis and is associated with the presence of NMDAR subunit 1 (NR1) antibodies ( 3). Although this was initially reported as unilateral cortical encephalitis, the presence of bilateral cortical involvement and meningeal inflammation in a subset of cases suggests a broader disease spectrum ( 2). The term “FLAIR-hyperintense lesions in anti-MOG-associated encephalitis with seizures” (FLAMES) was introduced by Budhram in 2019. The most common clinical manifestations of MOGAD are optic neuritis (ON), myelitis, and acute disseminated encephalomyelitis, while cortical encephalitis, demyelination of the brainstem and cerebellum, and progressive white matter damage are rare ( 1). MOG antibody-associated disease (MOGAD) is gradually becoming recognized as a new independent spectrum of disease. 
Myelin oligodendrocyte glycoprotein (MOG) is a protein expressed in the outermost layer of the myelin sheath of the central nervous system. However, FLAMES with bilateral medial frontal lobe involvement suggests the presence of the overlap syndrome. Over a mean follow-up period of 18.5 months, only one patient experienced residual visual impairment, while the remaining 11 patients had good prognoses.Ĭonclusion: FLAMES alone is difficult to distinguish from overlap syndrome based on clinical features. EEG showed slow waves in four cases, spike–slow waves in two cases, an epileptiform pattern in one case, and normal waves in two cases. Of the 12 patients, five showed lesions at other sites (e.g., the brainstem, corpus callosum, or frontal orbital gyrus) before or after the development of cortical encephalitis. Seven cases exhibited unilateral cortical FLAIR hyperintensity, and five cases (42%) had bilateral cortical FLAIR hyperintensity, including four cases involving the bilateral medial frontal lobes. The median CSF anti-NMDAR antibody titer was 1:10 (1:1–1:32), while the median serum MOG antibody titer was 1:32 (1:10–1:1024). Increases in intracranial pressure (median: 262.5 mmH 2O, range: 150–380 mmH 2O), cerebrospinal fluid (CSF) leukocyte count (median: 128×10 6/L, range: 1-610×10 6/L), and protein level (median: 0.48 g/L) were also observed. The most common clinical manifestations of FLAMES overlaid with anti-NMDARe were epilepsy (12/12), headache (11/12), and fever (10/12). Results: A total of 12 patients were analyzed in the study. Methods: We report a new case of this overlap syndrome and present a systematic review of similar cases in the literature to provide information on the clinical presentation, MRI features, EGG abnormalities, treatment, and prognosis of patients with this rare syndrome.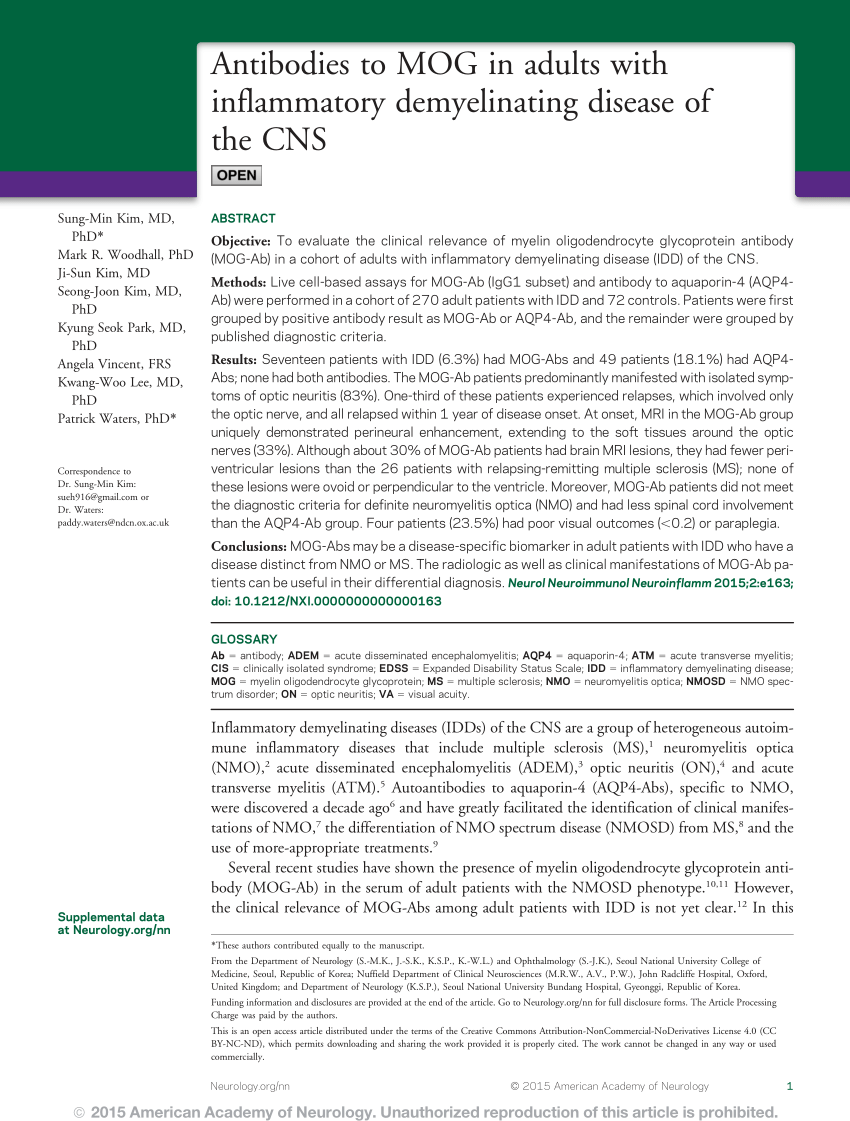  
However, this rare MOG antibody disease may coexist with anti-N-methyl-D-aspartate receptor encephalitis (anti-NMDARe), in an overlap syndrome with unknown clinical features and prognosis.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
